Associations between lifestyle score and participant characteristics
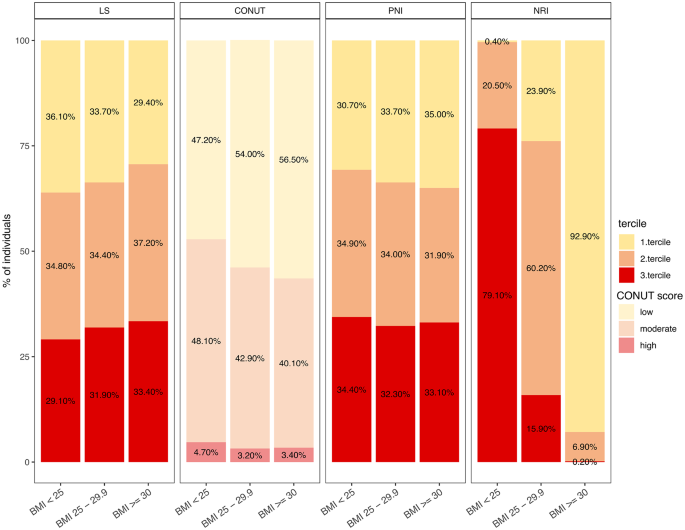
Overall, 6,073 participants (51.8% women, aged 56 ± 12 years,) have been included for our baseline lifestyle analysis with the major study characteristics being presented in Table 2. Sex distribution across the terciles (1st healthy, 2nd moderate, 3rd unhealthy LS) revealed 62.5% females and 37.5% males for the first tercile, whereas in the third tercile showed only 40.4% females and 59.6% males, demonstrating a relationship between lifestyle and sex (Supplemental Fig. 1b). We observed a decrease of age over the LS terciles (1st 57 ± 12; 2nd 55 ± 12 and 3rd 53 ± 11 years). Men consistently showed higher (i.e., less healthy) LS values across all age groups(Supplemental Fig. 1c). The average BMI was 27.28 ± 4.87 kg/m2 and demonstrated an increase in men across the LS terciles (Table 2) indicating a relatively healthy cohort. In line, the average total cholesterol level was 5.58 ± 1.07 mmol/L and low-density-lipoprotein (LDL) level at 3.51 ± 0.96 mmol/L, which were above the reference (> 5 mmol/L for total cholesterol and > 3 mmol/L for LDL) indicating a hypercholesterolemia. Although we observed no difference in LDL or total cholesterol across the LS terciles, high-density-lipoprotein (HDL) was significantly decreased over the terciles (1st; 2nd and 3rd mmol/l; p < 1 × 10–3, as determined by post-hoc Tukey’s test) indicating that an unhealthier lifestyle according to our LS, is associated with lower HDL levels. Figure 1 shows that 36.1% of underweight/normal-weight individuals are in the first tercile of the LS, while 33.4% of obese individuals are in the third tercile, representing the unhealthiest group. These proportions suggest a trend where individuals with lower BMI are more often classified in healthier terciles, and those with higher BMI in unhealthier terciles. However, the distribution closely aligns with random expectation, indicating that BMI alone does not strongly predict LS. Notably, 29.4% of individuals with a BMI > 30 kg/m2 are in the first tercile, demonstrating that higher BMI does not preclude healthier lifestyles. Similarly, some underweight/normal-weight individuals are in the third tercile, underscoring that lower BMI does not guarantee a higher LS. These findings highlight the LS’s ability to capture lifestyle behaviors across BMI categories, emphasizing the multifactorial nature of health behaviors.

The distribution of participants within respective terciles based on BMI [kg/m^2] categories—Underweight and Normal Weight (BMI = < 25), Overweight (BMI = 25–29.9), and Obesity (BMI = > 30)—is examined across the Lifestyle Score, CONUT Score, PNI, and NRI. The color coding is as follows: Yellow represents participants with a low lifestyle score or a mild risk of malnutrition (1st Tercile). Orange denotes participants with a moderately lifestyle score or a moderate risk of malnutrition. (2nd Tercile). Red indicates participants with a high lifestyle score or a high risk of malnutrition (3rd Tercile). For the CONUT Score, the tercile classification is challenging due to the low number of participants with high CONUT values, and thus the division is based on categories of low, moderate, and high risk. To reflect this, pale colors were used.
Association between the LS and the Framingham risk score
The average 10-year risk of coronary heart disease (CHD) in the LIFE-Adult cohort, based on the Framingham Risk Score (Supplemental Table 4), is approximately 7.4 ± 7.3%. This aligns with European Society of Cardiology data, placing the cohort in the low to moderate risk category26. The Spearman correlation coefficient between the LS and cardiovascular risk is 0.138, indicating a weak positive correlation; higher lifestyle scores are associated with higher cardiovascular risk (p = 4.2 × 10–27). Notably, we found a significant (p < 1 × 10⁻⁷) > 2% increase in the average FS for participants with unhealthier lifestyles (3rd tercile = 8.96%) compared to those with healthier lifestyles 1st tercile = 6.28%) (Fig. 2). Given that smoking is a component of both the LS and FS, we assessed the correlation between these scores excluding smoking to ensure it does not confound the observed relationships. When smoking was excluded from the LS, the correlation with cardiovascular risk substantially decreased and was no longer significant for Spearman’s rank correlation (ρ = 0.04, p = 0.06), while the Pearson correlation remained weak but significant (r = 0.05, p = 7 × 10–3). Among the individual components of the LS, Diet Score showed the strongest positive association with the FS, with significant correlations observed for both Spearman (ρ = 0.1, p = 2.14 × 10−8) and Pearson (r = 0.1, p = 6.5 × 10−9). Alcohol Score demonstrated a weak but significant positive correlation (Spearman: ρ = 0.05, p = 4 × 10–3; Pearson: r = 0.06, p = 4.2 × 10–4), whereas Physical Activity Score showed no significant correlation (Spearman: ρ = − 0.02, p = 0.3; Pearson: r = 9 × 10–3, p = 0.6).
In the illustration, the percentage risk of experiencing a cardiovascular event in the next 10 years is depicted based on the Framingham Score, stratified according to the terciles of the Lifestyle Score. The statistical significance of these differences was assessed using the t-test.
A healthier lifestyle is associated with a higher risk for malnutrition
Given that the majority of individuals in the LIFE-Adult cohort are categorized as normal or overweight (Table 2), it becomes interesting to investigate the prediction performance of LS terciles regarding malnutrition. However, all three tools, the CONUT, PNI, and NRI scores, indicate a very low to moderate risk for malnutrition across all three terciles in the LIFE-Adult cohort (Table 2).
Considering that CONUT scores of 0 indicate a low malnutrition risk, scores of 1 and 2 indicate a moderate risk, and scores equal to or greater than 3 indicate an increased risk of malnutrition, an average CONUT score of 0.69 across the LIFE-Adult cohort signifies a very low risk of malnutrition5,19. Unexpectedly, we observed a significant (p = 8 × 10–3) decrease of the CONUT across the lifestyle terciles (Table 2). Although, according to the CONUT all participants were well nourished, this suggests a lower likelihood of malnutrition especially in the unhealthy lifestyle group.
Cross-tabulation of LS and CONUT groups shows that most individuals in the 1st LS group (n = 1014, 49.4%) and 3rd LS group (n = 1109, 58.2%) fall into the low CONUT risk group, while only 3.2–3.6% are in the high-risk group. This distribution indicates a weak association between lifestyle behaviors and malnutrition risk, warranting further investigation (Table 3).
Similar to the CONUT score, according to the PNI the LIFE-Adult cohort was on average classified to have a moderate risk for malnutrition (55.18 ± 8.9, Tables 1, 2), with lower PNI scores indicating a higher risk for malnutrition, while higher scores suggest a lower risk (Table 1). Simultaneously to the CONUT score, we observed a significant decrease in the risk for malnutrition across our LS terciles (1st 54.9 ± 3.8; 2nd 55.1 ± 3.8 and 3rd 56 ± 16.7; p < 1 × 10–3; Table 2). However, it is noteworthy that within any lifestyle group, only a moderate risk for malnutrition could be identified, indicating the absence of a definitive severe risk. These findings suggest that the risk of malnutrition decreases with an unhealthier LS and higher average BMI values. However, both CONUT and PNI, consider only laboratory parameters regardless of the individual’s body weight.
In contrast, the NRI also incorporates individual’s body weight and similar to the PNI lower values indicate a higher risk of malnutrition (Table 1). Within the LIFE-Adult cohort we observed NRI scores ranging from 84.5 to 176.1 with an average value of 119.9 ± 9.6. Therefore, we again observed a moderate risk of malnutrition for each LS terciles (Table 2) with the highest values in the moderate (2nd tercile = 120.1 ± 9.7 and unhealthy living subgroups (3rd tercile = 119.76 ± 9.69), again probably indicating a lower risk for malnutrition in both groups.
Since LS already included diet we assessed correlations between diet in the LS and the malnutrition scores (Supplemental Table 6). Using Kendall’s τ, because of the discrete nature of the Diet score and the great number of ties in our datasets, we found correlations of 0.021 with the NRI, 0.030 with the PNI and − 0.002 with the CONUT score. The correlations between DietScore and NRI and PNI are statistically significant (p < 0.05). Interestingly, the smoking score shows either almost the same or a bigger correlation (− 0.03 for NRI, 0.08 for PNI and − 0.089 for CONUT).
In summary, all three scores assessing malnutrition observed either a mild or moderate risk within the LIFE-Adult cohort. Paradoxically, participants with healthier LS patterns showed relatively higher malnutrition scores, while those with less healthy lifestyles—who also had higher BMI on average—appeared at lower malnutrition risk (Table 2).
Association between the scores and MACE’s
The prevalence of CVD in the LIFE-Adult cohort, reported at 4.1%, should be interpreted with caution due to the limited evaluability of the anamnestic data. This is particularly relevant when compared to the 9.2% prevalence reported across Europe30.
However, albeit we expect the CVEs to be strongly underreported in the generally healthier LIFE-Adult cohort, both the CONUT-Score and the PNI revealed the highest percentage of cardiovascular events in their third tercile (Table 4). This indicates that the group with the highest susceptibility to malnutrition (3rd tercile) (The cut-offs for the population-specific terciles of the respective scores are presented in Table 1) also exhibits the highest prevalence of CVEs. In contrast the NRI score exhibits the lowest incidence of CVEs within the 3rd tercile, characterized by the highest risk of malnutrition. However, the NRI Score requires individual consideration since its formula included the individuals’ weight indicating that a higher weight corresponds to a higher NRI values but a lower risk for malnutrition. This indicates that the NRI may not be suitable for predicting CVEs in this cohort, further supported by the highest HDL and lowest triglyceride and total cholesterol levels in the third tercile (Supplemental Table 5).
Analysis of the mortality curves of LS, CONUT, PNI and NRI
To compare mortality hazard rates across different scores, we examined rates per score tercile (Fig. 3). Our LS did not show significant difference in the mortality rates between all three tercile (Fig. 3a). However, the survival curve for the third tercile is lower than that of the 1st and 2nd terciles, suggesting a higher overall mortality risk for those with least healthy lifestyle scores.
Mortality curves for all-cause mortality. X Axis: Months. LS = Lifestyle Score (Tercile 1 = LS: < 21; Tercile 2 = LS: 21–32; Tercile 3 = LS: > 32). CONUT-Score = Controlling Nutritional Status Score (Low = CONUT Score: 0; Moderate = CONUT Score: 1,2; High = CONUT Score: > = 3). PNI = Prognostic Nutritional Index. (Tercile 1 = PNI: > 56.35; Tercile 2 = PNI: 56.35–53.25; Tercile 3 = PNI: < 53.25). NRI = Nutritional Risk Index (Tercile 1 = NRI: > 122.8; Tercile 2 = NRI: 115.2–122.8; Tercile 3 = NRI: < 115.2).
While we did not observe a notable difference in mortality between the healthy (1st) and moderate (2nd) lifestyles, the unhealthiest group exhibited slightly higher mortality (Fig. 3a), consistent with the CVE prevalence in our cohort. Nevertheless, CONUT, PNI and NRI showed the highest mortality rate for the 3rd terciles with the highest malnutrition (p < 0.001, Fig. 3b–d). Additionally, men and individuals with high smoking scores experienced significantly elevated mortality risks (Supplemental Fig. 2a, b).
To elucidate the impact of malnutrition and lifestyle on mortality, four Cox regression models were analyzed. The effects of the four scores on mortality, adjusted for sex, age, BMI, and MACE, are shown in Table 5.
The LS yielded a hazard ratio (HR) of 1.01 (95% CI 1.00–1.03, p = 0.02), indicating an increase in mortality risk. Individuals in the 1st tercile had a lower HR of 0.71 (95% CI 0.50–1.02, p = 0.056) compared to the 3rd tercile, suggesting a potential but not significant lower risk, while the 2nd tercile showed a significant lower risk (HR 0.68, 95% CI 0.48–0.96, p = 0.028).
Among the LS sub scores, only the Smoking Score was significantly associated with increased mortality risk (HR 1.02, 95% CI 1.00–1.05, p = 0.024). The Diet, Physical Activity, and Alcohol Scores showed no significant associations (Supplemental Fig. 3).
In comparison, the CONUT Score (HR 1.27, 95% CI 1.16–1.39, p < 0.001) was significantly associated with higher mortality risk, supported by significantly lower HRs for the 1st (HR 0.40, 95% CI 0.29–0.55, p < 0.001) and 2nd (HR 0.46, 95% CI 0.34–0.62, p < 0.001) terciles. The PNI (HR 1.00, 95% CI 1.00–1.01, p = 0.139) and NRI (HR 0.91, 95% CI 0.89–0.94, p < 0.001) showed a lower overall effect on mortality, with lower malnutrition terciles indicating a significantly reduced mortality risk (Table 5).
Analysis of age–dependent association between lifestyle score and mortality
A significant LS–age interaction was observed (likelihood-ratio test p = 0.037). Using the standardized Lifestyle Score (LS_z; higher values indicate a less healthy lifestyle), each 1-SD increase in LS was associated with an adjusted HR for all-cause mortality of 1.11 (95% CI 0.84–1.46) in participants < 60 years and 0.97 (0.76–1.23) in those 60–69 years—neither statistically significant—whereas in participants ≥ 70 years the HR was 1.55 (1.23–1.95). Consistently, within the ≥ 70-year stratum, risks relative to the healthiest tercile (T1) were HR 1.99 (1.08–3.68) for T2 and HR 2.80 (1.51–5.21) for T3. Overall, poorer lifestyle was most strongly associated with higher mortality in older participants, while associations in younger groups were weaker and not statistically discernible, likely reflecting fewer events and limited power. (Fig. 4).
Panel A: Adjusted hazard ratios (HRs) for all-cause mortality per 1-SD higher (worse) Lifestyle Score (LS_z) within age strata (< 60, 60–69, ≥ 70). Models are Cox proportional hazards adjusted for sex and BMI; points show HRs and whiskers 95% CIs on a log scale (n and number of events shown per stratum). The LS_z × age-group interaction was significant (likelihood-ratio test p = 0.037). Panel B: Among participants aged ≥ 70 years, adjusted HRs comparing LS terciles to the healthiest tercile (T1): T2 vs T1 and T3 vs T1. Models are Cox proportional hazards adjusted for sex and BMI; points show HRs and whiskers 95% CIs on a log scale.
Longitudinal changes in lipid profiles across lifestyle terciles
Analyses were restricted to participants with paired measurements (n = 2,530; baseline 2011–2014, follow-up 2018–2021; ≈7 years apart). Across all LS terciles, total and HDL cholesterol declined over time, whereas triglycerides increased. Paired Wilcoxon signed-rank tests indicated statistically significant within-person increases in triglycerides in each tercile, with the largest median rise in T3 (least healthy). Decreases in total and HDL cholesterol were modest overall and slightly more pronounced in T1 (healthiest). Exact estimates and p-values are reported in Table 6.
link